Realizing the Promise of All-Payer Claims Databases
Editor’s Note: America spends more on health care per person than any other developed country, only to have the lowest life expectancy among them. Despite our expenditures—now one out of every five dollars of national income—our system’s shortcomings are abundant. Nearly half of American adults have difficulty affording care, and four in ten report delaying or forgoing care due to cost. Racial and ethnic health disparities in our country are pervasive and newly compounded by COVID-19. And in a system where coverage is often linked to employment, in the first months of the public health emergency, an estimated 14.6 million workers and their family members lost their employer-sponsored insurance.
In a fragmented system of care regulated by a patchwork of federal and state entities, too often we do not have a comprehensive and cohesive view of how our systems of health are performing and where they are failing—a prerequisite for developing effective and targeted solutions for the systems’ shortcomings. We survey the damage and often place the burden of assessing and fixing the systems’ gaps on states. But to solve national issues, we need national solutions—or at a minimum, coordinated state action.
In a new white paper, summarized below, Manatt Health proposes actions that the federal government can take in partnership with states to strengthen our local and national health data capacity to support evidence-based policymaking. Policymakers, researchers, purchasers and consumer advocates may use this new health data capacity to better understand and address cross-state health system challenges and establish a common, data-based foundation on which future reforms and actions may be shaped and evaluated. Click to download a free copy of the full white paper; to view our recent “National Health Data Summit” webinar on demand; and to access our full library of materials to help you better understand, plan for and implement all-payer claims databases (APCDs). And be sure to register for the next webinar in our series—“State Health Data Organizations: Engines of Market Transparency and Insight.”
In 2020, health care spending in the United States increased by nearly 10% to reach $4.1 trillion, or 20% of the U.S. economy. Yet, for an industry powered by data and foundational to the health and well-being of our nation, policymakers, regulators and other public stakeholders often lack comprehensive, cohesive and timely information about its operations and performance.
Reflecting our nation’s fragmented health care delivery system and its patchwork of federal and state regulatory authorities, our nation’s health system data is also siloed, scattered and incomplete. State insurance departments, Medicaid departments, Affordable Care Act (ACA) Marketplaces and state employee health benefit programs, for example, each collect and monitor data for the plans, providers and individuals under their respective authorities, providing each a relatively narrow view into the dynamic markets they serve.
To address local information gaps, state policymakers and regulators from across the country—and across the political spectrum—have invested in APCDs, which can offer unique insights into local market dynamics and operations.
State APCDs
State APCDs are market-wide repositories of public and private payer health care claims and encounter data, including records of health care service payments that provide contextual information about the individuals served and their diagnosed conditions. Eighteen states currently have APCDs, and at least six others have an APCD in development.
State APCDs can provide users with broad and longitudinal cross-payer insights into health system performance and changing population health. Policymakers use them to inform health care and payment reform design as well as to support market transparency. State APCDs have been used to:
- Create and monitor baseline statistics of state health insurance coverage, service utilization, service costs, cost trends and health outcomes
- Identify inequities in health system access and use as well as disparities in health condition prevalence and outcomes
- Support regulatory oversight of payers and providers
- Identify health system failures to inform policy responses
- Facilitate an understanding of whole-person health needs by linking data for individuals covered by more than one payer and bridging health and social service/public health data sources
- Provide purchasers, payers and consumers with health service cost and quality information to make informed health coverage purchasing and network design decisions
By 2025, at least half of all states, including the nation’s four largest, will have an operating APCD. However, the current state APCD operating model was not intended to serve as a national health data blueprint and has several limitations that prohibit important local and national use cases.
Opportunities to Enhance State APCD Use and Usefulness
Presently, state APCD agencies collect membership, claims and provider data from national and local health care payers licensed to operate in their markets and for which they have regulatory authority or voluntary cooperation to collect such information (Exhibit 1). Payer data is collected, as often as monthly, in five to nine different files and in accordance with each state’s data collection standards, practices and processes. Files may comprise tens of millions of records, which states must review for integrity before linking them with previously received data to create a longitudinal dataset. Each state pursues its own APCD research and reporting priorities using the data it receives.
Exhibit 1: Current State APCD Operating Model
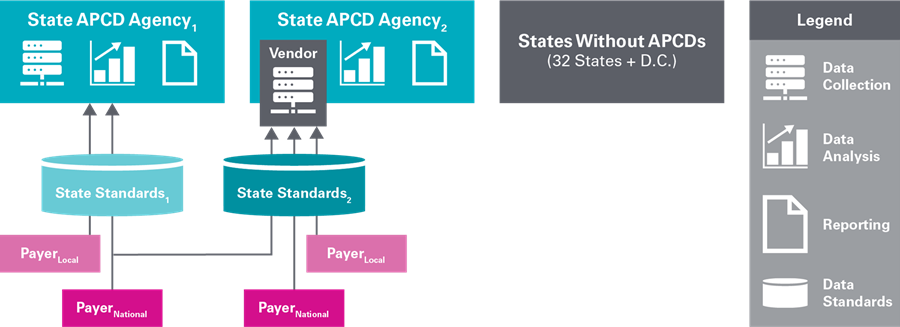
While state APCDs have demonstrated their capabilities to provide state policymakers and regulators, among other data users, with deep insights into local markets, the current state operating model has several limitations that can constrain their use and usefulness:
- Missing data for key populations and services
- Inconsistent data collection and access requirements
- Need for sustainable and adequate funding for state health data capacity
With more than half of states not having an APCD, national data collection gaps limit national, regional and cross-state analyses and benchmarking and result in new state health information inequities among states.
Developing a New National APCD Operating Model
Throughout 2022, more than 40 federal and state policymakers, regulators, researchers and other health data leaders were engaged to confirm the legal, regulatory, technical and operational root causes of these state APCD limitations and to design and test potential alternative APCD operating models that could resolve them—to the benefit of current and future state APCD users.
Stakeholders identified and assessed a number of alternate APCD operating models and recommended a model that would strengthen and build from the existing state-based APCD structure to create new national health data capacity: the “Federally Facilitated State Data Partnership” model (Exhibit 2). In this model, states would continue to serve as APCD data owners and have the option of participating in a national health data compact. As part of the compact, states would continue to collect payer data locally but in alignment with new national data standards and practices. States would then share collected data with a new national health data organization (HDO). In exchange for their participation, states would receive federal financial support and be granted new access to federally regulated and administered health data, such as data for the ERISA-preempted self-insured. For states without an APCD or that choose not to participate, the national HDO would collect APCD data directly from payers operating in those states to complete a national picture. The national HDO would provide national policymakers, regulators and researchers—as well as states—with a new, centralized resource for cross-state health system administrative data.
The national HDO would be contracted and funded by, but sit outside, the federal government and be governed by a combination of federal, state and consumer privacy representatives in a public and transparent manner. The national HDO governing body would be responsible for overseeing the organization and its operations as well as approving national APCD data standards, baseline privacy and security standards, and the purposes for which the national APCD may be accessed and used.
Exhibit 2: Proposed National APCD Model: Federally Facilitated State Data Partnership
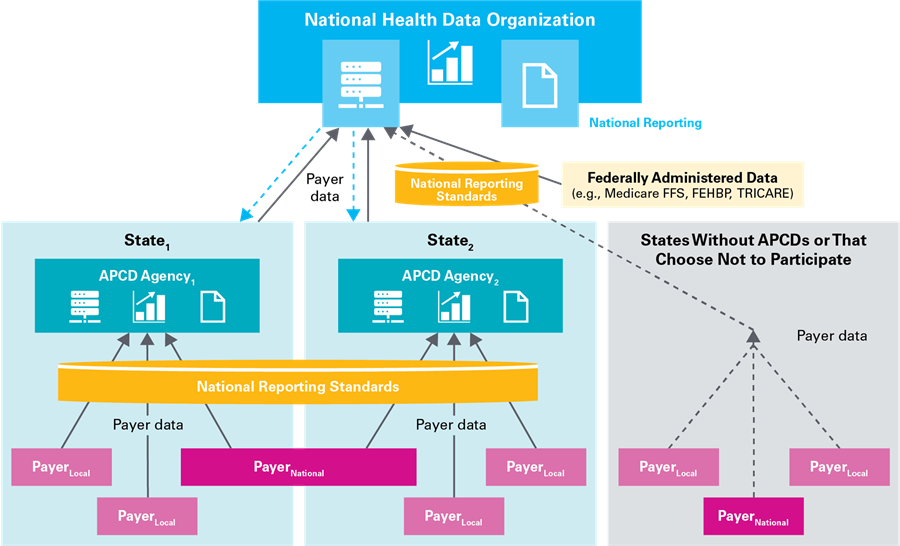
The model would create new national and cross-state data access, comparability and analytic capacity while preserving state APCD data ownership.
Establishing a Federal and State APCD Action Plan
States cannot support APCD system change alone despite state data submitters, collectors and users benefiting from the more complete data—and the stronger local analytic capacity—that would result. Federal leadership and sustained partnership are required to realize a national APCD model that strengthens state health data infrastructure, incentivizes cross-state data harmonization, and builds the centralized data collection, analysis and governance capacity needed to support a national, coordinated system of administrative health data reporting and use.
The effective implementation of the recommended national APCD operating model will require federal and state stakeholders to work together to establish:
- A national HDO that is viewed as a trustworthy, independent and protective steward of the nation’s health care administrative data
- A federal-state-consumer governance partnership to oversee and direct national HDO activities
- A plan to resolve self-insured reporting barriers to ensure states have access to the data necessary to oversee their markets and purchasers (and other users) have data to compare across markets
- A source of federal health data funding for states to support model implementation and sustain permanent and robust state or regional health data collection and analytic infrastructure
- A national compact on APCD data privacy and security to set baseline data privacy and security protections for the national HDO and participating states.
Establishing a national, coordinated APCD operating model would provide state HDOs with new data access and funding support, enhancing the value they can provide to local stakeholders; reduce the reporting burden for multistate payers; and improve access to critical information about our health care system nationally. National, regional and cross-state analytics and benchmarking would become possible and could be employed across states to foster health system transparency and accountability, monitor and respond to public health needs, and inform health care priorities and investment strategies.
Federal and state leaders now have the opportunity to recast our nation’s APCD model to provide policymakers and regulators, purchasers, consumers, and researchers with the health system data and resources they need to counterbalance historical information inequities with one of America’s largest, most critical, and most data-driven industries and to foster a more transparent and competitive market.
1 “How does health spending in the U.S. compare to other countries?” Peterson-Kaiser Family Foundation (KFF) Health System Tracker, January 21, 2022. Accessed July 25, 2022. Available .
2 “How does U.S. life expectancy compare to other countries?” Peterson-KFF Health System Tracker, September 28, 2021. Accessed July 25, 2022. Available .
3 “National Health Expenditure Data,” Centers for Medicare & Medicaid Services (CMS).
4 “Americans’ Challenges with Health Care Costs,” KFF, July 14, 2022. Accessed July 27, 2022. Available .
5 “Achieving Racial and Ethnic Equity in U.S. Health Care,” The Commonwealth Fund, November 18, 2021. Accessed July 27, 2022. Available .
6 “COVID-19 Cases and Deaths by Race/Ethnicity: Current Data and Changes Over Time,” KFF, February 22, 2022. Accessed July 27, 2022. Available .
7 “Update: How Many Americans Have Lost Jobs with Employer Health Coverage During the Pandemic?” The Commonwealth Fund, January 11, 2021. Accessed July 27, 2022. Available .
8 “National Health Expenditure Data,” CMS. Accessed May 25, 2022. Available .
9 This paper focuses on health system administrative data, claims, and encounters and records of services rendered to patients by providers, which typically include additional information on patient diagnoses and payment amounts between payers and providers.
10 For example, see Colorado’s Center for Improving Value in Health Care’s (CIVHC) state cost analysis: “Total Cost of Care Multi-State Analysis,” CIVHC, February 2018. Available . Also see: “Healthcare Procedure Cost Drivers,” Maine Health Data Organization. Accessed May 25, 2022. Available .
11 For example: “HPC DataPoints, Issue 22, Growth in Out-of-Pocket Spending for Pregnancy, Delivery, and Postpartum Care in Massachusetts,” Health Policy Commission (HPC), March 29, 2022. Accessed August 15, 2022. Available .
12 For more examples of potential Medicaid APCD use cases, see: “Recommendation Report for Expanded Access to the Minnesota All-Payer Claims Database: Initial Findings – Appendix D,” Minnesota Department of Health (MDH), February 2022. Accessed May 25, 2022. Available .
13 For example, the Utah Department of Health’s Office of Health Care Statistics (OHCS) used the Utah APCD to assess provider payment variation for colonoscopies, a commonly considered “shoppable service.” It found that payments around its median price ranged by 400%, “demonstrat[ing] that selecting a low-cost provider may be possible” with minimal research. “Exploring the Cost of Colonoscopy in Utah July 2019 through June 2020,” Utah Department of Health, OHCS, March 23, 2021. Accessed May 25, 2022. Virginia Health Information (VHI), which stewards the Virginia APCD under the authority of the Virginia Department of Health, used its APCD to quantify the volume and costs of preventable ED visits in the state, finding that “about 10% of the 1.1 million ED visits in 2020 may have been potentially avoided and treated with lower cost care in a [primary care practitioner’s] office” while generating health system savings of nearly $67 million. “Potentially Avoidable ED Visits in 2020,” VHI, May 2, 2022. Accessed May 25, 2022. Available .
14 Massachusetts’ APCD was used as the backbone for the state’s opioid use disorder analysis in 2017: “An Assessment of Fatal and Nonfatal Opioid Overdoses in Massachusetts (2011 – 2015),” Commonwealth of Massachusetts, August 2017. Accessed May 25, 2022. Available .
15 For example, Massachusetts’ CHIA supports payer/provider price transparency initiatives through its Compare Treatment Costs tool and broader bulk releases of procedure price data. For more information, see: “CompareCare,” Commonwealth of Massachusetts. Accessed May 25, 2022. Also see: “Bulk Release of Procedure Price Data,” CHIA. Accessed May 25, 2022. Also see: “CompareMaine,” Maine HDO. Accessed May 25, 2022. Available .
