L.A. City and County COVID-19 Weekly Update (December 21, 2020)
COVID-19 Rates Continue to Rise Dangerously
Last week, Los Angeles County (the County) experienced the highest daily numbers of new COVID-19 deaths, cases and hospitalizations ever reported throughout the pandemic. At a press conference on Wednesday, December 16, 2020, County Director of Public Health Dr. Barbara Ferrer described the current situation as an “explosive and very deadly surge” and called on all Angelinos to stay home and avoid potentially spreading the virus as much as possible. She also noted that, at the current rate, an average of two Angelinos are dying of COVID-19 per hour.
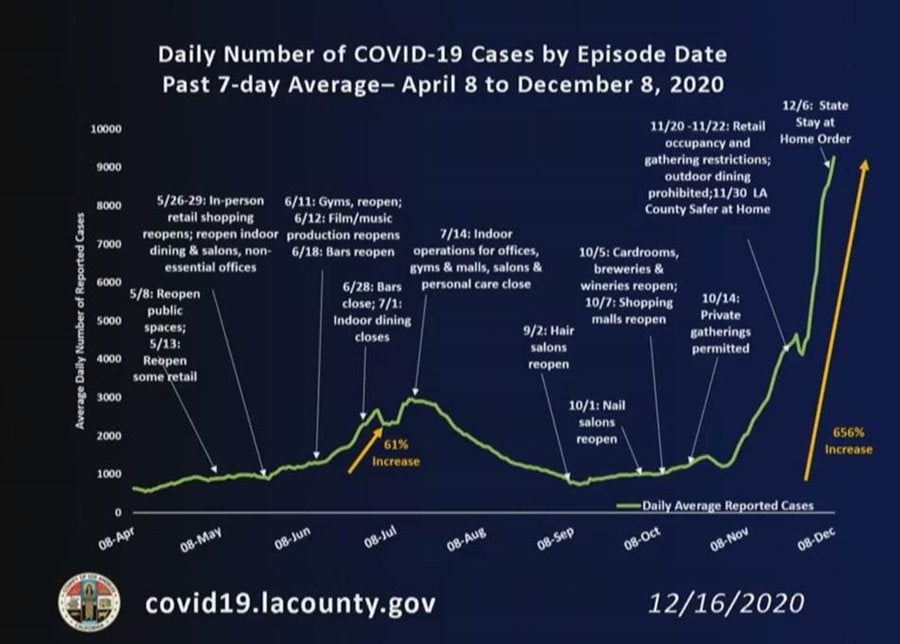
Dr. Ferrer noted several alarming statistics:
- Average new cases have gone from ~6,000 per day in November to almost 10,000 per day now
- Test positivity rates have nearly quadrupled
- Since November 9, average daily deaths have increased nearly 600%, from an average of 12 deaths per day to more than 70 per day last week
- The County is now experiencing average new case numbers that are almost four times the levels seen in the last week of November
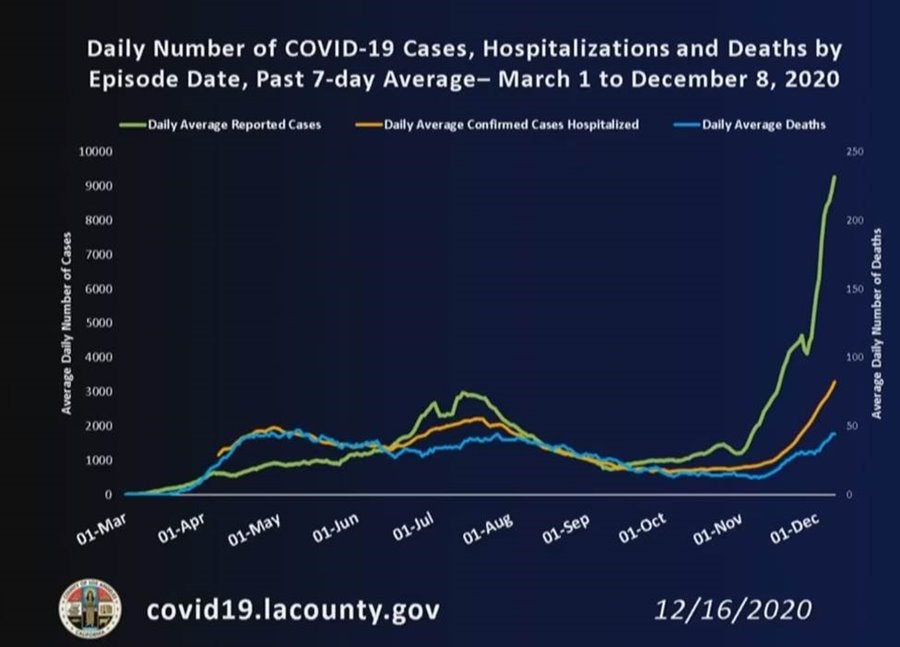
Dr. Ferrer also explained that, because hospitalizations typically follow two weeks after infection, and deaths two weeks after that, the County anticipates hospitalization and death rates to continue to rise for the next several weeks.
Over the course of last week, the County’s cumulative test positivity rate rose a full percentage point, from 12% on Sunday, December 13, to 13% on Thursday, December 17. In comparison, the test positivity rate had remained at 7% for most of the year, but had been at 11% as of Friday, December 11.
The County remains in Tier 1 of the state’s Blueprint, along with 55 of the state’s 58 counties, covering more than 99% of the state’s population.
Hospital Capacity
Last week, hospital capacity in the County dropped precipitously. As of Wednesday, December 16, the County’s hospital demand model indicated that the County’s effective transmission rate was 1.20, or 1 in every 80 residents. On Thursday, December 17, the state projected that the Southern California region’s ICU capacity was 0.0%. On Friday, December 18, there were fewer than 100 ICU beds available County-wide.
At a press conference on Wednesday, December 16, County Director of Health Services Dr. Christina Ghaly issued the starkest warning to date about the County’s COVID-19 situation, stating, “Our hospitals are under siege, and our models show no end in sight … the worst is ahead of us.” She indicated that the hospital system in the County is not able to provide the appropriate level of care for all patients (COVID-19 and non-COVID-19) due to demand. Dr. Ghaly also said that a continued surge may result in the rationing of care, particularly ICU care.
The County’s situation is projected to be “dire” at least through January. The number of ICU patients could exceed the number of licensed ICU beds in the County (2,500) in the coming weeks, even accounting for additional hospital flexibility and emergency measures. Dr. Ghaly also indicated, for the first time, that the County’s EMS system is becoming overloaded, resulting in delays in triage and treatment for emergent patients.
Vaccinations
On Monday, December 14, County hospitals began administering the first doses of the Pfizer vaccine. According to the County Department of Public Health press release.
The first shipment of vaccine arrived today at one of nine pre-positioned sites, with the remaining eight sites receiving their shipment over the next two days. The current expected initial allocation for L.A. County is 82,875 doses, and we are hoping to receive two additional allocations in December. This does not include allocations for the Cities of Long Beach and Pasadena, which have their own independent health departments and are receiving their own allocations.
The nine prepositioned sites have been working with the Los Angeles County Department of Public Health (Public Health) and EMS to make arrangements to redistribute vaccine so that every acute care hospital that serves COVID-19 patients receives a pro-rata share of this initial allocation. Public Health has been hosting webinars, holding office hours, and distributing information in order to help prepare all the acute care hospitals for this large undertaking.
A second allocation of the vaccine that should arrive later this month will allow for a distribution of vaccines to all health care personnel and residents at our skilled nursing facilities, along with continued distribution to frontline healthcare and EMS personnel.
