Closing the Digital Health Disconnect: A Blueprint for Optimizing Digitally Enabled Care
Editor’s Note: In a new report, summarized below, the American Medical Association (AMA) and Manatt Health explore the digital health disconnect and propose opportunities for health care stakeholders to address it. The report also highlights the AMA’s commitment to resolving the disconnect and empowering physicians in their journey to achieve the promise of digitally enabled care. The findings and opportunities featured in the report were gathered through a series of in-depth interviews and workshops with a wide range of physicians, patients, health plans, employers, health systems, investors, digital health companies and digital health experts. To download your free copy of the full report, click here.
Catalyzed by the COVID-19 pandemic, we have entered an era of digitally enabled care—fully integrated in-person and virtual care models that hybridize care delivery based on clinical appropriateness and other factors, such as convenience and cost. This evolution toward digitally enabled care, explored within the AMA’s Return on Health report, is transforming how we think about accessing, providing, managing and paying for health care.
Building on rapidly accelerating levels of investment in the digital health space over the past decade, the COVID-19 pandemic forced the widespread adoption of digital health tools. Health care organizations are increasingly designing and implementing omnichannel digitally enabled care offerings and integrating new virtual care solutions. Physicians, many of whom had reservations about telehealth prior to the pandemic, have found the experience of delivering care virtually to be quite positive. Digital health companies have entered the market at a record pace.
Despite record levels of venture funding, new company creation and virtual care adoption, however, there are few clear signs that the digital transformation of health care is meaningfully improving access, outcomes, quality, care experience, clinician experience or health equity.
In an ideal world, in-person and digitally enabled care models would be integrated and harmonized to amplify the value of health care and deliver effective, whole-person care. Yet often, digital health products exist in silos and risk additional fragmentation, higher costs, and diminishing patient and provider experiences. The “digital health disconnect” is the chasm between the theoretical potential that digitally enabled care models promise and the reality of “parallel” care that predominates today.
Defining the Digital Health Disconnect
Despite growing investment in digital health companies over the past decade, the digital health industry is still nascent, and its funding is a fraction of that for the broader health care industry. A significant share of digital health funding from 2012 to 2019 was directed to “first generation” digital health companies, which often designed and sold products focused on wellness, urgent care and low-acuity primary care to health plans and employers. We are now moving into the “second generation,” where companies are designing solutions that deliver or enable the delivery of more complex services and have a more diversified range of business models. It is still early in the digitally enabled care evolution, but this new era’s companies offer the potential to truly augment and enhance in-person care, as well as address issues of access, quality and equity. At the same time, if the models of care are not well connected, there is risk of negatively impacting continuity of care and the patient-physician relationship.
To fully realize the potential of digitally enabled care and appreciate the drivers of the digital health disconnect, we have sought to understand the range of stakeholder perspectives on how the digital health industry has evolved over the past ten years. Though stakeholder perspectives varied, nearly all agreed that to close the digital health disconnect, we must avoid perpetuating the failures of today’s health care system, including:
- Lack of patient, family and physician centricity in care model design. With few exceptions, care models are designed to meet the operational needs of complex health care delivery organizations, federal and state regulatory requirements, and payers’ billing rules. Rarely are care models designed and implemented with sufficient patient and physician input.
- Care fragmentation. Fragmentation between health care providers is a perpetual failing of our current health care system and often leaves patients, or their families and caregivers, with the responsibility of trying to coordinate care across multiple care settings.
- Data silos. Data sharing between health care delivery organizations is a persistent challenge. As of 2018, only 48% of office-based physicians could electronically exchange patient health information outside of their organizations, and only 31% could integrate outside electronic health information into their own electronic health record (EHR) systems.
- Overly complex payment models that disincentivize high-value care. Despite the move to and proliferation of value-based payment models in Medicare, Medicaid and the commercial market, these models are often overly complex and burdensome to implement. Research highlights that few impact cost, quality and equity as intended.
- Asking too much of overburdened physicians. Physician burnout affects more than three in five physicians, and one in five physicians intends to leave practice in the next two years.
- Too slow to scale effective care models. On average, it takes 17 years for new biomedical innovations to translate “from bench to bedside.” We need to rapidly reduce the time it takes for evidence-based digitally enabled care models to proliferate.
A Blueprint for Optimizing Digitally Enabled Care
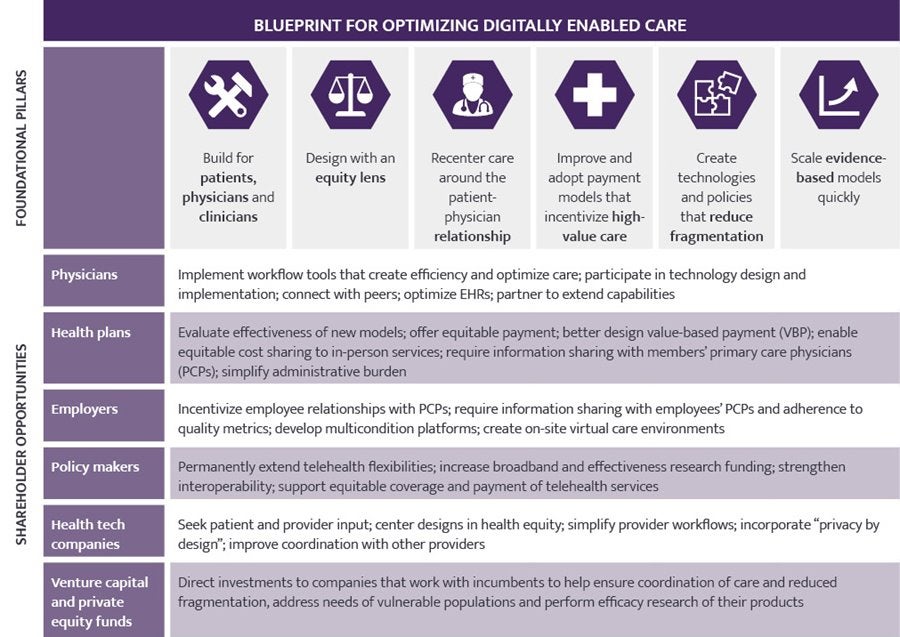
Addressing the digital health disconnect will take time, resources, policy redesign, and a commitment by all stakeholders to build care models and companies differently than we have in the past. This will be health care’s next great challenge and will progress iteratively given the incredible scale and complexity of the health care industry. Through our research, the AMA and Manatt have designed a blueprint to address the digital health disconnect and achieve optimized digitally enabled care. The blueprint is summarized below.
Stakeholder Opportunities
Achieving the promise of digitally enabled care requires health care stakeholders to move in partnership. Following are opportunities for stakeholders to contribute to the full realization of digitally enabled care.
Opportunities for physicians
- Implement digital health tools that enhance the workflow to create efficiencies, reduce administrative burden and optimize patient care.
- Actively participate in the design, evaluation and implementation of new technologies using human-centered design approaches.
- Connect with your peers to learn about what is, and what is not, working for them.
- Optimize and utilize the full functionality of existing EHR systems, leverage new laws that empower physicians as EHR technology consumers, and put processes in place for continuous EHR optimization.
- Pursue partnerships with other providers and companies that allow clinicians to extend practice capabilities while maintaining the primacy of the patient-physician relationship.
Opportunities for health plans
- Share outcomes data from digitally enabled care models.
- Use claims data to more rigorously evaluate and rapidly scale digitally enabled care models.
- Support providers in transitioning to digitally enabled care by ensuring coverage parity and equitable payment for virtual care and designing processes that do not increase administrative burden.
- Ensure copayments, coinsurance and deductibles for virtual services are not higher than for equivalent in-person services.
- Better design value-based payment models in collaboration with providers and patients.
- Impose requirements on contracted virtual care providers to share patient encounter data with members’ primary care physicians.
- Allow all contracted physicians to provide care via telehealth to their patients.
- Evaluate, review and significantly limit the volume of prior authorizations that impede patient care.
Opportunities for employers
- Incentivize employees to establish and maintain a regular source of primary care, and ensure those clinicians are appropriately compensated for virtual care.
- Require that any contracted digital health companies share patient encounter data (and ideally, proactively coordinate care) with employees’ primary care physicians, and report on/adhere to quality and cost metrics.
- Accelerate the development of high-quality, multicondition digital health platforms that also deliver or are closely linked with primary care.
- Create safe and private environments to enable on-site virtual care.
Opportunities for policymakers
- Permanently extend telehealth coverage policies that were adopted temporarily during the COVID-19 public health emergency.
- Expand funding to study and scale digitally enabled care models.
- Increase federal broadband funding, outreach and education to achieve affordable broadband access and digital literacy for every American.
- Update, focus and enforce information sharing rules to address technical, contractual and financial roadblocks.
- Support coverage of telehealth on the same basis as in-person care, equitable payment for virtual care, and narrow exceptions to licensure for out-of-state physicians providing ongoing care to an existing patient via telehealth.
Opportunities for health tech companies
- Seek clinician and patient input on the design of new digital health tools.
- Ensure that new digitally enabled care models are always developed with a health equity lens.
- Build solutions that simplify workflows for clinicians and caregivers and save money and time for practices.
- Incorporate a “privacy by design” approach in the development of digital health tools to ensure patients’ data are protected.
- Improve coordination of care with other health tech companies and predominantly brick-and-mortar providers (especially primary care physicians).
- Build integrated referral relationships with brick-and-mortar health care organizations to support patient access to comprehensive virtual and in-person care.
Opportunities for venture capital and private equity funds
- Increase investment in companies that are committed to working with incumbent health care organizations.
- Direct investments to more diverse founders and to companies that address the needs of vulnerable populations.
- Prioritize investment in companies that perform high-quality research studies of the efficacy of their products and services.
- Look for opportunities to drive healthy consolidation in a manner that reduces fragmentation and promotes comprehensive patient care models.