Ensuring Children’s Access to Care Using Telehealth in Medicaid During COVID-19
The COVID-19 pandemic is wreaking serious health and economic consequences on children and families. At the same time, pediatric providers have scaled their telehealth capabilities at warp speed to reduce disease spread and ensure children and adolescents, especially those with special healthcare needs, continue to receive needed care. State Medicaid programs have a wide range of policy levers available to increase or restrict access to telehealth services generally. This article, based on our recent webinar, summarizes those policy levers and highlights the pediatric telehealth services that are of particular relevance for children with special healthcare needs. To view the full webinar—presented by Manatt Heath, the American Academy of Pediatrics, Family Voices, and the Georgetown University Center for Children and Families—click here.
Pediatric Telehealth Visits Have Increased 15-Fold During the Pandemic
In the period before the COVID-19 pandemic, telehealth adoption among pediatricians was limited. According to a survey from the American Academy of Pediatrics, only 15% of pediatricians had reported using telehealth prior to COVID-19, with insufficient payment and inability to bill for services the main barriers to adoption.1 Actual utilization of telehealth among the pediatric population was less than 1% of overall volume—meaning more than 99% of visits were still conducted in person.2 In late March, early in the pandemic, weekly ambulatory visits for individuals of all ages declined nearly 60% from pre-COVID-19 levels. While they have been slowly recovering since then, they are still below the baseline.3
Pediatrics experienced the greatest decline in visits during COVID-19 relative to other specialties. Even as visits for other specialties have begun to recover, pediatric ambulatory volume is still significantly down from pre-COVID-19 levels.4 This decrease corresponds to a similar drop in childhood vaccination rates, especially among children older than 24 months of age.5
Since March, across specialties, telehealth visits have increased as in-person ambulatory visits have dropped. When we look specifically at pediatrics, we can see telehealth utilization soaring across the United States. As noted above, prior to the COVID-19 pandemic, telehealth visits represented less than 1% of overall pediatric visits. By April, pediatric telehealth usage had spiked to more than 15% nationally, with utilization higher in urban areas than in rural areas. Pediatric diagnostic data shows that more than half of telehealth visits in April were for behavioral health and developmental disorder diagnoses.6
Pediatric Telehealth Offers Both Benefits and Challenges
Pediatric telehealth offers many important benefits. It can increase access to primary and behavioral healthcare, as well as to specialty care—particularly during the pandemic when social distancing restrictions are in place. In addition, telehealth reduces the burden on families related to unnecessary travel and time off work. It also ensures patient safety during the pandemic, and it enables providers to observe and interact with children and families in their homes, where they are often more comfortable.
Along with its benefits, however, telehealth can present some notable challenges. Obviously, it is not possible to administer immunizations or conduct a comprehensive hands-on physical exam via telehealth. In addition, children and families may have trouble accessing telehealth due to broadband or other technological limitations. It also may be hard to engage with some children or family members via video—and privacy may be a concern, particularly for the adolescent population. Finally, families may not have experience using telehealth or may perceive it to be lower quality than in-person care.
Inequities in Access to Telehealth Persist
COVID-19 has put a spotlight on the significant inequities in access to telehealth for low-income families. These inequities are exacerbated for rural residents, racial/ethnic minorities, older adults, those with limited health literacy and those with limited English proficiency. Consider that only 56% of low-income Americans have broadband access at home;7 only 71% of Americans own a smartphone, with lower rates among low-income Americans;8 and only 53% of low-income Americans have basic digital literacy.9 While telehealth has the potential to improve access to care, significant challenges remain for Medicaid beneficiaries in accessing virtual care services.
Medicaid Is a Critical Driver of Pediatric Telehealth
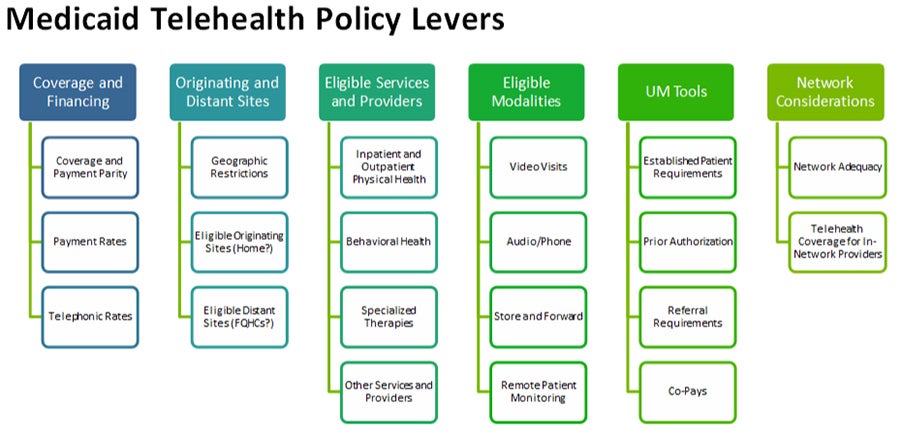
State Medicaid programs have a wide range of policy levers available to increase or restrict access to telehealth services generally. These fall under six main categories—coverage and financing, originating and distant sites, eligible services and providers, eligible modalities, utilization management tools, and network considerations, as outlined in the figure below. For example, within coverage and financing, states can decide whether they will pay for telehealth services at the same rate as the equivalent in-person service (i.e., payment parity) and what the rates will be for telephonic services. With respect to eligible modalities, Medicaid programs can decide which specific modalities (e.g., video, phone, remote patient monitoring) will be covered.
Most state Medicaid programs have expanded access to at least some pediatric telehealth services in response to the pandemic. A subset of pediatric telehealth services is of particular relevance for children with special healthcare needs. In many cases, state Medicaid programs have issued specific guidance related to coverage of the following services:10
- Well-Child Services: Certain components of a well-child visit cannot be performed via telehealth (e.g., comprehensive physical exam, hearing and vision exams, immunizations); however, having telehealth as an option for children older than 24 months of age to deliver some preventive components of the well-child visit during times when in-person care is not possible (e.g., during a future state of emergency) can improve access to well-child care. To date, 19 states and Washington, D.C., have issued guidance related to Medicaid coverage of well-child services during the COVID-19 pandemic.
- Specialized Therapies (Physical, Occupational, Speech Language): In some states, specialized therapies were already covered by Medicaid when delivered via telehealth; however, the pandemic has pushed many other states to expand telehealth coverage to include these services. Telehealth has been an important tool to help some children continue critical specialized therapy treatments remotely without disruption to their routine. To date, 38 states and Washington, D.C., have issued guidance related to Medicaid coverage of specialized therapy services during the COVID-19 pandemic.
- Early Intervention Services: For infants and children ages 0–3, telehealth can be a challenging mode of care delivery and is often not appropriate for delivery of services within an early intervention program. Some states, however, have chosen to enable a select set of early intervention services to be delivered via telehealth during the pandemic, such as care management/coordination, training and counseling. Going forward, states may choose to carve out select services that may be appropriately delivered via telehealth in order to enhance care coordination and reduce the burden (e.g., unnecessary travel, time off work) on families enrolled in these programs. To date, 16 states have issued guidance related to Medicaid coverage of Early Intervention services during the COVID-19 pandemic.
- Children’s Behavioral Health Services: Most state Medicaid programs covered the delivery of behavioral healthcare services for children via telehealth prior to COVID-19. In response to COVID-19, many states expanded their telehealth-eligible behavioral health offerings to include services such as Applied Behavioral Analysis. In addition, some states have opted to allow providers to deliver services, including behavioral health services, via audio-only visits as opposed to video visits. This flexibility has helped increase access for those who may have issues accessing the Internet and broadband. To date, all states have issued guidance related to Medicaid coverage of behavioral health services during the COVID-19 pandemic.
Looking Ahead
While every state Medicaid program has temporarily expanded its coverage of telehealth services to some degree in response to the COVID-19 pandemic, states are now in the process of determining which changes to make permanent in order to maintain access to care via telehealth for children beyond the pandemic period. We expect Medicaid programs to use the various policy levers outlined in this article to continue to calibrate telehealth coverage post-pandemic to be more expansive, in general, than pre-pandemic, but likely less expansive than coverage has been during the pandemic period.
1 Blake Sisk et al., Pediatrician Attitudes Toward and Experiences With Telehealth Use: Results From a National Survey (Academic Pediatrics, July 2020).
2 FAIR Health, July 2020. Data provided to Manatt for the purposes of the webinar.
3 Ateev Mehrotra et al., The Impact of the COVID-19 Pandemic on Outpatient Visits: Practices Are Adapting to the New Normal (The Commonwealth Fund, June 2020).
4 Ibid.
5 Santoli JM, Lindley MC, DeSilva MB, et al. Effects of the COVID-19 Pandemic on Routine Pediatric Vaccine Ordering and Administration — United States, 2020. MMWR Morb Mortal Wkly Rep 2020;69:591–593.
6 FAIR Health, July 2020. Data provided to Manatt for the purposes of the webinar.
7 Pew Research Center. Internet/Broadband Fact Sheet. Accessed August 26, 2020.
8 Pew Research Center. Mobile Fact Sheet. Accessed August 26, 2020.
9 Nouri, S, Khoong, E, et al. Addressing Equity in Telemedicine for Chronic Disease Management During the Covid-19 Pandemic. NEJM Catalyst. May 4, 2020.
10 Manatt Health. Executive Summary: Tracking Telehealth Changes State-by-State in Response to COVID-19. August 21, 2020.
