States Are Leveraging Medicaid Waivers to Transform Their Behavioral Health Systems
Introduction
As the nation experiences unprecedented levels of behavioral health needs—even further exacerbated by the COVID-19 pandemic—state Medicaid programs have increasingly looked for flexibility to craft services and payment models that support improved access and outcomes. As the single largest payer for behavioral health services nationwide, Medicaid is in a unique position to impact millions of Americans’ access to quality behavioral health care. To engender this effort, the Centers for Medicare & Medicaid Services (CMS) has waived historical restrictions on inpatient substance use and mental health services and permitted states to leverage Section 1115 demonstrations to support broad-based reform.
Background on Substance Use Disorder and Serious Mental Illness/Serious Emotional Disturbances Waivers
Institutions for Mental Disease Waivers for Substance Use Disorders
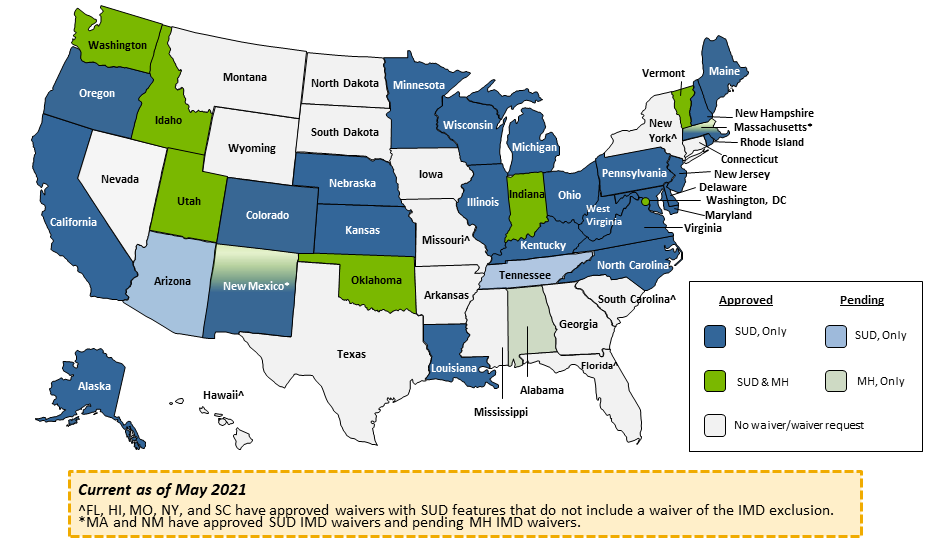
Over the last five years, 32 states (see Figure 1) have obtained federal waivers of the institutions for mental disease (IMD) exclusion—the historical prohibition on using federal Medicaid funds to pay for treatment delivered to individuals ages 21 to 64 residing in institutions with more than 16 beds—for individuals receiving substance use disorder (SUD) services. In November 2017, CMS released a state Medicaid director (SMD) letter—replacing July 2015 guidance—notifying states of the opportunity to design Section 1115 demonstrations focused on SUDs. In the SMD letter, CMS advised states that they could apply to waive the IMD exclusion if they met key conditions, including providing access to SUD treatment across critical levels of care, increasing use of evidence-based SUD treatment and placement criteria to ensure individuals are placed at the appropriate level of care, introducing SUD provider quality standards, and strengthening care coordination for individuals with SUDs. These demonstrations have solidified Medicaid’s role as the largest source of coverage and funding for substance use prevention and treatment in the country, covering nearly 40 percent of adults with an opioid use disorder (OUD) and 17 percent of adults experiencing any type of addiction. Since the first state waivers were approved in late 2015 and 2016, expanding access to evidence-based SUD treatment across all levels of care remains a critical need due to continued rise in drug use and overdose deaths.
IMD Waivers for Serious Mental Illness & Serious Emotional Disturbance
In recent years, CMS and states have taken an integrated approach to treating mental illness and SUD to effectively address rising behavioral health (BH)—mental health (MH) and SUD—needs. Nearly half of the 19.3 million adults with SUD have a co-occurring mental illness, and 18 percent of adults with mental illness have a co-occurring SUD. In November 2018, CMS released another SMD letter notifying states of the opportunity to design Section 1115 demonstrations focused on adults with a serious mental illness (SMI) and children with a serious emotional disturbance (SED). In the SMD letter, CMS advised states that they could similarly apply to waive the IMD exclusion for individuals obtaining care for serious MH conditions if they ensure the quality of inpatient and residential care; improve care coordination and care transitions; improve access to a continuum of care for MH treatment; and promote earlier identification of and engagement in MH care. To prevent over-institutionalization of individuals with SMI/SED, states must meet additional requirements, including maintaining their current funding for outpatient community-based MH services and adhering to a 30-day average length of stay in IMDs.1 A growing number of states—seven with approved waivers and three with pending waivers as of May 2021—are pursuing waivers of the IMD exclusion for SMI/SED.
Figure 1. States With Approved or Pending Waivers of the IMD Exclusion
Key Features of SUD and SMI/SED Section 1115 Demonstrations
In addition to waiving the IMD exclusion for SUD and MH treatment, states are using Section 1115 demonstrations to implement a range of strategies to improve care for Medicaid enrollees with BH needs.
Additional Treatment and Recovery Services
A number of states are using waiver authority to cover or pilot a range of BH treatment and recovery services, many of which can be covered via Medicaid State Plan authority, and link these services to waivers of the IMD exclusion. States commonly use Section 1115 IMD-focused waivers to cover SUD and MH treatment and detoxification services, particularly residential levels of care that are often provided in IMDs. Other states like Illinois and Washington, D.C., are using their Section 1115 demonstrations to cover or pilot crisis intervention and mobile crisis response services—a move that may become increasingly more common among states once the American Rescue Plan (ARP) Act community mobile crisis intervention services option—which allows states to cover qualifying services using Medicaid State Plan or Section 1115, 1915(b) or 1915(c) authorities—becomes effective in April 2022.2
A significant number of states with Section 1115 BH-focused demonstrations are using their waivers to cover peer support services, which use the lived experience of individuals recovering from SUD to support others in treatment and recovery, for individuals with SUD and/or SMI. Of the 37 states covering peer supports for individuals with SUD, most are covering this service using Medicaid State Plan authority. Peer support services can be provided in a range of clinical and non-clinical settings, and as a complement to or replacement for clinical treatment, including for crisis response services.
Additionally, states use their Section 1115 BH demonstrations to provide enhanced home and community-based services (HCBS) to individuals with SMI, SED and/or SUD. In recognition that individuals with BH needs account for approximately one-third of all homeless individuals, states like Washington, Illinois, Florida and Hawaii are providing supportive housing benefits to adults with SUD and/or SMI who are or at risk of becoming homeless. In addition to Section 1115 waiver authority, states can cover supportive housing services through Section 1915(c) or 1915(i) authority. These supportive housing and tenancy support services assist beneficiaries with a range of services including securing appropriate housing, building relationships with landlords and neighbors and obtaining the skills necessary to manage a household.
Targeted Delivery System Reform With Behavioral Health Components
Several states also use waiver authority to obtain Medicaid funding to pursue delivery system and payment reforms targeted to specific populations, including those with BH needs. A shrinking number of states operate Delivery System Reform Incentive Payment (DSRIP) programs with BH components, which provide states with significant funding to help providers, especially hospitals, invest in delivery system reform.3 For example, Washington’s DSRIP program, authorized through a Section 1115 demonstration in 2017, includes waivers of the IMD exclusion for SUD and SMI/SED, as well as projects targeted toward the integration of physical and behavioral health services and strategies to address SUD and projects focusing on SUD and projects focusing on physical health and BH integration. It will be critical to watch whether the Biden Administration reverses the course set out by the Trump Administration, which was gradually phasing down DSRIP programs in an effort to shift Medicaid programs toward more sustainable value-based purchasing integrated into Medicaid delivery systems. Under the Trump Administration, states were still able to leverage Medicaid funding for and pursue BH-focused delivery system and payment reforms using 1115 waivers other than DSRIP waivers. For example, Hawaii, Massachusetts and North Carolina obtained Medicaid funding through broader Section 1115 demonstrations for health-related initiatives addressing social determinants of heath for specific populations, including those with BH needs.
Coverage Expansion for Individuals With Behavioral Health Needs
Select states also use Section 1115 authority to extend either limited or full Medicaid coverage to adults and children with SED, SMI or SUD who are otherwise ineligible for Medicaid. For example, Rhode Island uses its 1115 demonstration to expand Medicaid eligibility to children with SED who require treatment in a psychiatric residential treatment facility and do not meet income requirements for Social Security Income. The state also provides a limited benefit package to uninsured adults with incomes from 133–200 percent of the federal poverty level who have a mental illness or SUD.
Looking Ahead
As the first state-focused IMD demonstrations come up for renewal and more than 60 percent of states gain experience operating these demonstrations, federal and state governments have an opportunity to take stock of these demonstrations. Key questions to watch in the months ahead include:
- How effective have SUD demonstrations been at increasing SUD treatment and leading to reductions in overdose deaths?
- Will CMS accelerate approval of SMI waivers?
- What pressures may emerge for additional protections against over-institutionalized care as more states begin to seek such waivers?
- What efforts will be made to integrate MH and SUD treatment via Section 1115 demonstrations?
- Will states integrate child-focused BH reforms into these waivers that have long focused on adults with BH needs?
- How will CMS bring its strong focus on equity into these waivers going forward?
As BH care needs among Americans change, it is essential that CMS and state Medicaid agencies remain nimble and innovative.
1 States may not claim Medicaid matching funds for any part of an IMD stay for mental health that exceeds 60 days.
2 The ARP Act enacted on March 11, 2021, establishes a state option to provide community mobile crisis intervention services for a five-year period beginning in April 2022. As an incentive to state adoption, the law provides for an 85 percent enhanced federal matching rate for qualifying services for the first three years of state coverage.
3 Thirteen states originally had DSRIP waivers with 12 approved by the Obama Administration and one—Washington—approved by the Trump Administration in 2017.
